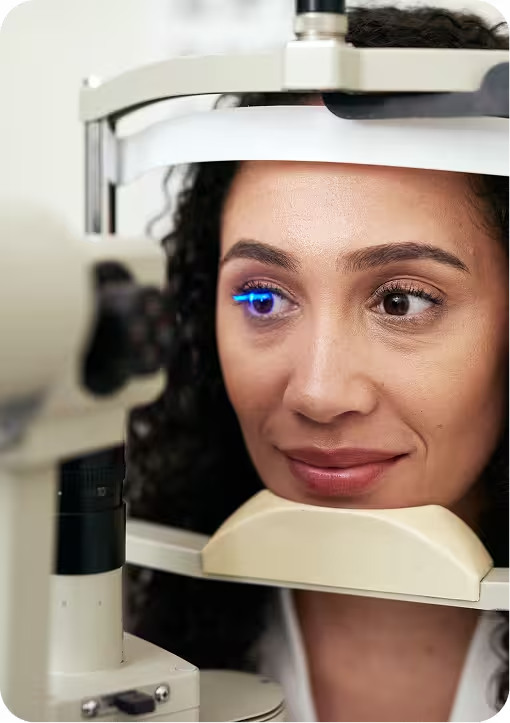
Performance-Driven Billing
Ophthalmology Billing Consultants
ECBC provides the highest level of personal service with the most experienced ophthalmology billing specialists, using advanced technology and deep industry expertise to maximize collections and ensure accurate, compliant eye care billing—so providers can focus on their patients.
Ophthalmology Billing Services
Ophthalmology Practice Management Starts with a Dedicated Account Manager.
The medical billing specialist assigned to your account will check all charges for accuracy and completeness.
Denial management in medical billing is the most important aspect of what we do.
ECBC offers a medical accounts receivable management service to help Ophthalmology practices maximize their profits.
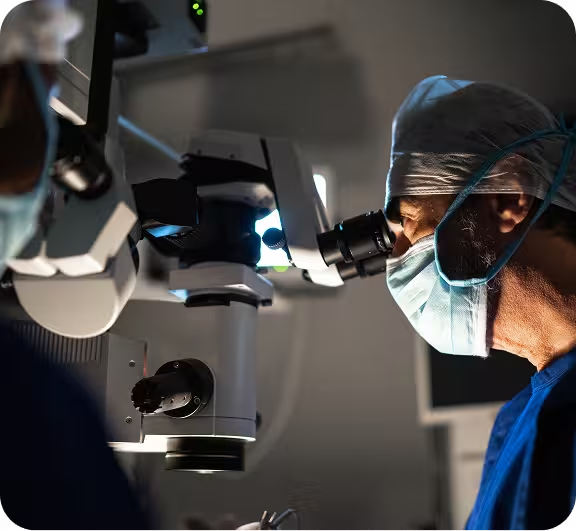
Eye Care Billing Consultants (ECBC) provides comprehensive, ophthalmology-focused revenue cycle management through an experienced in-house team of ophthalmic billers, coders, and account managers. We manage every aspect of your billing—from claims and coding to denials, EOBs, and collections—helping improve cash flow, reduce administrative burden, and maximize reimbursement. With deep specialty expertise and a personalized approach, ECBC delivers reliable results and peace of mind so you can stay focused on patient care.
HEAR FROM OUR CLIENTS

Ophthalmology Practice Tips
Understanding Medical vs. Vision Insurance Billing
Understanding the difference between medical and vision insurance billing is critical for eye care practices. Patients are often confused…
Best Practices for Insurance Verification in Eye Care Offices
Insurance verification is essential for preventing billing issues in eye care practices. Confirming both medical and vision benefits before…